HEALTH
Is Ambien Addictive?

Ambien, known generically as zolpidem, is a medication commonly prescribed for the short-term treatment of insomnia. While it can be effective in helping individuals fall asleep, questions surrounding its potential for addiction have become increasingly prominent. Understanding the nature of Ambien, its effects, and the risks associated with its use is essential for anyone considering this medication.
What is Ambien?
Ambien belongs to a class of medications called sedative-hypnotics. It works by affecting neurotransmitters in the brain, particularly gamma-aminobutyric acid (GABA), which plays a crucial role in promoting sleep. By enhancing the effects of GABA, Ambien helps to induce sleep more quickly and improve overall sleep quality. This mechanism of action is particularly beneficial for those who struggle with insomnia, as it targets the brain’s natural sleep pathways to facilitate a more restful night.
Ambien is often considered a go-to solution for acute insomnia, but it is essential to understand that it does not address the underlying causes of sleep disturbances. Factors such as stress, anxiety, and lifestyle choices can contribute to sleep issues, and while Ambien may provide temporary relief, it is advisable for users to explore comprehensive strategies for long-term sleep health. This might include cognitive behavioral therapy for insomnia (CBT-I), relaxation techniques, or lifestyle changes aimed at improving sleep hygiene.
How is Ambien Used?
Typically, Ambien is prescribed for short-term use, often for a duration of one to two weeks. It is intended for individuals who have difficulty falling asleep or staying asleep. The medication is usually taken just before bedtime and is available in immediate-release and extended-release formulations, allowing for flexibility based on individual sleep patterns. The immediate-release form is designed to help users fall asleep quickly, while the extended-release version can assist those who have trouble staying asleep throughout the night, providing a more sustained release of the medication.
It is crucial for patients to follow their healthcare provider’s instructions regarding dosage and duration of use. Taking Ambien for longer than recommended can lead to dependence, tolerance, or withdrawal symptoms upon discontinuation. Additionally, users should be aware of potential interactions with other medications or substances, such as alcohol, which can exacerbate side effects and increase the risk of adverse reactions.
Common Side Effects
While Ambien can be effective, it is not without side effects. Commonly reported side effects include drowsiness, dizziness, and headache. Some individuals may also experience more severe reactions, such as memory loss or unusual behavior while asleep, including sleepwalking or engaging in activities without full awareness. These side effects can raise concerns about the safety and long-term implications of using Ambien. Users are often advised to avoid driving or operating heavy machinery until they know how the medication affects them.
In rare cases, individuals may experience complex sleep-related behaviors, such as preparing and eating food, making phone calls, or even driving while not fully awake. Such incidents can pose significant risks not only to the user but also to others. Therefore, it is essential for anyone considering Ambien to have a thorough discussion with their healthcare provider about the potential risks and benefits, as well as to explore alternative treatments that may be more suitable for their specific situation. Monitoring and open communication with a healthcare professional can help mitigate risks and ensure safer use of this medication.
The Risk of Addiction
One of the most pressing concerns regarding Ambien is its potential for addiction. Although it is not classified as a traditional narcotic, it does have properties that can lead to dependence in some individuals. Understanding how addiction can develop is crucial for anyone considering this medication.
Physical Dependence vs. Psychological Dependence
Addiction can manifest in different forms, primarily physical and psychological dependence. Physical dependence occurs when the body adapts to the presence of a drug, leading to withdrawal symptoms when the drug is not taken. Psychological dependence, on the other hand, involves a compulsion to use the drug despite negative consequences.
With Ambien, physical dependence can develop, especially when used for extended periods or at higher doses than prescribed. Individuals may find that they need to take more of the medication to achieve the same sedative effects, leading to a cycle of increased use.
Signs of Addiction
Recognizing the signs of addiction is vital for early intervention. Common indicators include:
- Increased tolerance to the medication, requiring higher doses to achieve the same effect.
- Experiencing withdrawal symptoms when not taking Ambien, such as anxiety, insomnia, or irritability.
- Using the medication for purposes other than prescribed, such as to cope with stress or emotional issues.
- Neglecting responsibilities or relationships due to the time spent obtaining or using the drug.
Factors Influencing Addiction Risk
Not everyone who takes Ambien will develop an addiction. Several factors can influence the likelihood of dependence, including genetics, mental health history, and personal circumstances.
Genetic Predisposition
Research indicates that genetic factors can play a significant role in addiction. Individuals with a family history of substance abuse may be at a higher risk of developing dependence on medications like Ambien. Understanding one’s genetic background can provide insight into potential vulnerabilities.
Co-occurring Mental Health Disorders
Many individuals who struggle with insomnia may also experience mental health disorders such as anxiety or depression. Those with underlying mental health issues may be more susceptible to developing an addiction to Ambien as they may use the medication to self-medicate. Addressing these co-occurring conditions is crucial for effective treatment and reducing the risk of dependence.
Safe Use of Ambien
For those who are prescribed Ambien, it is essential to use the medication safely to minimize the risk of addiction. Following a few guidelines can help ensure responsible use.
Follow Prescribing Guidelines
Always adhere to the prescribing physician’s guidelines regarding dosage and duration of use. Avoid increasing the dose without consulting a healthcare professional, as this can lead to dependence.
Monitor Usage
Keeping track of how often and how much Ambien is taken can help individuals stay aware of their usage patterns. If there are signs of increased tolerance or dependence, it is crucial to seek help promptly.
Alternatives to Ambien
For individuals concerned about the risk of addiction, there are alternative treatments for insomnia that can be considered. These options may include lifestyle changes, behavioral therapies, and non-addictive medications.
Lifestyle Changes
Implementing healthy sleep habits can significantly improve sleep quality. This may include maintaining a consistent sleep schedule, creating a restful sleep environment, and avoiding stimulants like caffeine close to bedtime. Regular exercise and relaxation techniques, such as meditation or deep breathing, can also promote better sleep.
Cognitive Behavioral Therapy for Insomnia (CBT-I)
CBT-I is a structured program that helps individuals identify and change thoughts and behaviors that contribute to insomnia. This evidence-based approach has shown effectiveness in treating sleep disorders without the use of medication.
Conclusion
While Ambien can be an effective short-term solution for insomnia, the potential for addiction is a valid concern. Understanding the risks, recognizing the signs of dependence, and exploring alternative treatment options are essential steps for anyone considering this medication. Open communication with healthcare providers can help ensure safe and effective management of sleep issues, ultimately leading to healthier sleep patterns and improved overall well-being.
If you or a loved one is grappling with the challenges of insomnia and the potential risks of Ambien addiction, Northern Illinois Recovery Center is here to offer support. Nestled in the tranquil surroundings of Crystal Lake, IL, our JAHCO-accredited facility provides a comprehensive range of services, including detox, residential, and various outpatient programs, all tailored to foster successful recovery. Recognized by Newsweek as one of the nation’s top providers and driven by our conviction that recovery is within reach, we pride ourselves on outcomes that surpass industry standards. Don’t let addiction control your life. Contact Us today to begin your journey to better sleep and overall well-being.
HEALTH
How Preventive Dental Care Shapes Lifelong Oral Health

Achieving and maintaining a healthy smile is much more than a cosmetic concern. Oral health serves as a vital foundation for one’s overall wellness by influencing numerous aspects of daily life, from nutrition to self-confidence. Preventive dental care offers a pathway to protecting your teeth and gums against disease and infection. With routine dental checkups and proper home care, people can help avoid future dental complications, potentially costly treatment, and maintain strong oral health for years to come. For those considering restorative options, learning about affordable dental implants can also be a valuable step towards improving their dental health and quality of life.
Investing in preventive care not only leads to brighter smiles but also supports long-term health. Taking proactive steps, such as adopting consistent oral hygiene habits and seeking regular dental visits, empowers individuals to catch issues early. This approach helps reduce risks for more complex procedures and supports lasting comfort and well-being.
The Importance of Regular Dental Check-Ups
Routine appointments with a dental professional serve as a crucial line of defense against serious oral health concerns. Dental checkups typically involve a thorough examination of the teeth and gums, professional cleanings, and sometimes diagnostic X-rays to uncover hidden concerns. When issues like early-stage cavities or the beginning signs of gum disease are found, dentists can provide prompt and effective treatment, helping patients avoid more advanced dental conditions or expensive interventions down the road.
Daily Oral Hygiene Practices
Maintaining optimal oral health begins with simple habits practiced every day. Brushing at least twice daily with fluoride toothpaste and flossing once a day are fundamental components of any preventive routine. These actions help to remove plaque, a film of bacteria, setting the stage for tooth decay and gum disease. Supplementing brushing and flossing with an antimicrobial mouthwash can further reduce bacteria and contribute to fresher breath.
Fluoride Treatments and Dental Sealants
Fluoride is well known for its ability to strengthen tooth enamel, offering vital protection against cavities. While fluoride is commonly added to public water supplies, some individuals may benefit from additional fluoride treatments during dental visits, particularly children, adolescents, and those with heightened cavity risk. Dental sealants provide another effective preventive strategy. By applying a thin, protective layer to the chewing surfaces of molars, sealants can block out food and bacteria, significantly lowering the likelihood of tooth decay among children and teens.
Healthy Diet and Lifestyle Choices
What you consume can have a lasting impact on your dental health. A diet packed with fresh produce, lean proteins, and whole grains delivers essential nutrients that keep teeth and gums resilient. Reducing your intake of sugary foods and beverages helps guard against cavities. Habits such as avoiding tobacco and limiting alcohol use are also critical for preventing oral cancers and supporting ongoing dental health.
Addressing Dental Anxiety
Many individuals experience unease or even fear when visiting the dentist. Dental anxiety can impede the pursuit of necessary preventive care, potentially leading to neglected oral health. Open communication with your dental provider about your concerns is vital. Modern dental offices offer solutions from sedation dentistry to relaxation and coping techniques. These options can transform the dental experience, making it easier to attend regular visits and receive needed care with greater comfort.
The Link Between Oral and Overall Health
Oral health extends beyond the mouth, with research increasingly revealing links to wider systemic conditions. Issues such as poor gum health and untreated cavities have been associated with increased risks for heart disease, diabetes, and respiratory infections. Conversely, diligent oral hygiene can help protect against these serious health concerns. A recent study reported by Fox News highlighted that maintaining a simple and consistent brushing routine may also contribute to reducing dementia risk and other related conditions.
Overcoming Barriers to Preventive Care
Despite the clear benefits, obstacles like financial constraints, lack of transportation, or limited education about oral health can prevent individuals from receiving regular care. Community-based programs, mobile dental units, and sliding-fee structures have emerged to address these challenges and make services more accessible. Public awareness campaigns and outreach efforts are also essential to educate people about the importance of preventive dental care and the resources available to them. For example, initiatives discussed in a World Health Organization article demonstrate how targeted strategies can improve oral health outcomes in local communities.
Adopting a proactive approach to preventive dental care sets a foundation for lifelong oral health. Through regular dental visits, dedicated home care, and mindful lifestyle habits, everyone can work toward a confident smile and enhanced well-being at every age.
HEALTH
What to Know Before Getting Dental Implants
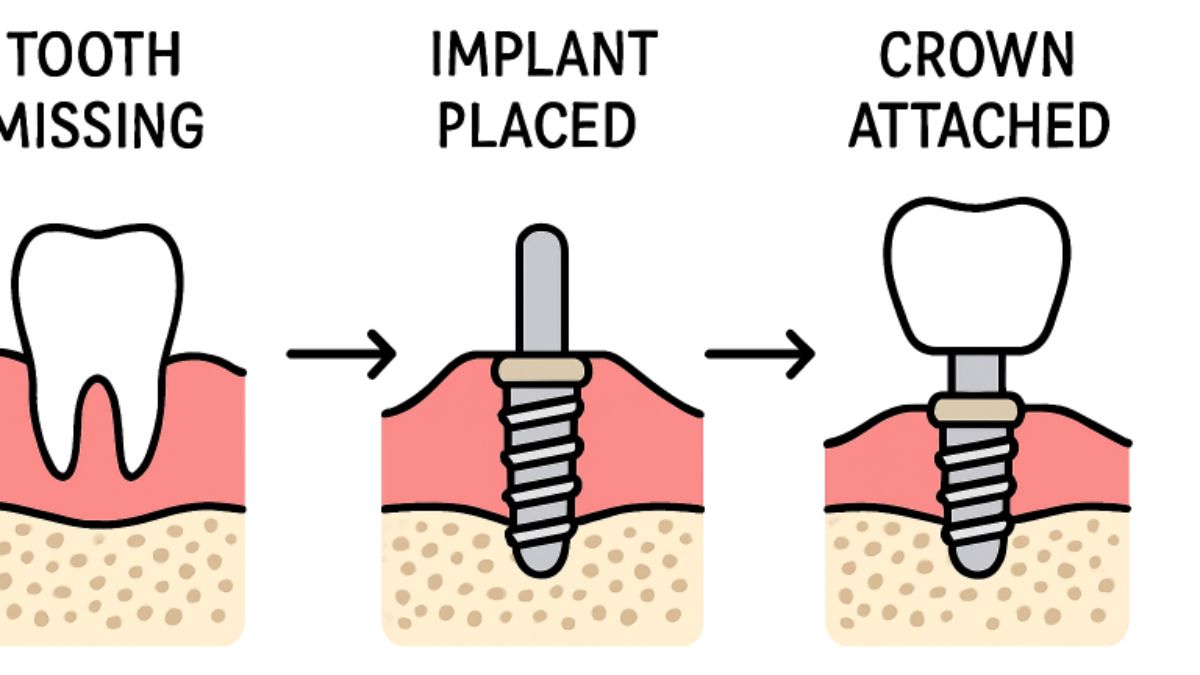
Dental implants have transformed restorative dentistry by providing a durable, comfortable, and natural-looking solution for replacing missing teeth. Many individuals are considering options such as denture implants to regain their confidence and oral function. However, questions often arise regarding implant procedures, candidacy, potential risks, and costs. Understanding clear answers to these questions can help you make a decision that’s right for your dental health. When deciding between dentures and implants, it’s important to understand what each treatment involves, the recovery time required, and which option best fits your specific needs and lifestyle. Dental professionals frequently address concerns about pain, longevity, daily maintenance, and how implants compare to traditional options. If you’re considering dental implants, obtaining accurate, up-to-date information is crucial for a smooth treatment experience and satisfying results.
What Are Dental Implants?
Dental implants function as artificial tooth roots, typically made from medical-grade titanium. These posts are surgically placed into the jawbone, where they integrate with your bone tissue in a process called osseointegration. After the implant is stable, a connector and a custom crown are attached, resulting in a secure, natural-looking tooth replacement. Dental implants are customized to match the color and shape of your natural teeth, ensuring a seamless blend within your smile.
Who Is a Suitable Candidate for Dental Implants?
Candidates for dental implants need healthy gums, no untreated dental conditions, and sufficient jawbone density to support the dental implant post. Factors such as smoking, uncontrolled diabetes, or ongoing periodontal disease can negatively impact healing and the success of the procedure. Before treatment, your dentist will conduct a thorough screening to ensure that implants are a safe and effective option for you.
What Does the Implant Procedure Involve?
The procedure for placing dental implants involves several stages, each crucial for the long-term success of your new teeth:
- Initial Consultation: Your dental provider will evaluate your oral health, review your medical history, and take digital scans or X-rays to assess jawbone strength.
- Surgical Placement: The titanium post is surgically positioned within the jawbone under local anesthesia. This step forms the stable foundation for your future restoration.
- Healing and Osseointegration: Over several months, the implant fuses with your jawbone, a vital process that ensures stability and prevents bone loss.
- Abutment Placement: After healing, a small connector (abutment) is attached to the implant to hold the crown in place.
- Crown Attachment: A custom-made crown is affixed to the abutment, completing the restoration and restoring full function and appearance.
How Long Do Dental Implants Last?
Dental implants are designed for longevity and, with proper care, can last a lifetime. The implant itself is typically permanent, though the crown may need to be replaced after 10 to 15 years due to normal wear. Consistent oral hygiene, avoiding smoking, and regular dental visits all contribute to the long-term success of dental implants.
Are Dental Implants Painful?
Most patients find dental implant procedures less uncomfortable than anticipated. During surgery, local anesthesia minimizes pain, and any post-operative discomfort is usually mild and short-lived. Over-the-counter pain medications or prescribed analgesics are generally effective during the initial healing period. After a few days, most individuals can return to their usual routines without significant discomfort.
What Are the Advantages of Dental Implants?
- Durability: Implants can last for several decades if cared for properly, making them a cost-effective, long-term solution.
- Natural Appearance: The design of implants mimics real teeth in both look and function, giving a seamless, attractive smile.
- Bone Preservation: By stimulating jawbone growth, implants prevent the bone loss commonly seen after tooth extraction.
- Enhanced Chewing Function: Unlike removable dentures, implants allow you to eat a wide variety of foods with confidence.
These benefits often give dental implants an edge over traditional bridges or dentures, especially for those seeking lifelong oral health improvements.
What Are the Potential Risks or Complications?
While dental implant success rates are high, complications can occur. Risks include infection around the implant site, implant failure (rare but more likely in smokers), injury to nerves near the jaw, or sinus issues with implants placed in the upper jaw. Choosing a skilled dental specialist, following post-care instructions, and maintaining excellent oral hygiene are the best ways to minimize these risks. For detailed information on potential risks, refer to the FDA’s guidelines on dental implants.
How Much Do Dental Implants Cost?
The overall price of dental implants depends on the number of implants needed, the type of restoration, pre-existing oral health conditions, and location. Typically, one implant with a crown will cost between $3,000 and $5,000. Dental insurance plans may partially cover the expense, but many policies still categorize implants as elective or cosmetic. Discussing options with both your provider and insurer can clarify out-of-pocket expenses and payment plans.
Conclusion
Dental implants are a reliable, innovative solution for restoring missing teeth and enhancing your oral health, function, and confidence. Knowing what to expect before, during, and after the procedure will help you make a decision tailored to your unique needs. For all individual considerations, work closely with a trusted dental professional who can guide you through the process and help achieve lasting results.
HEALTH
Bilieter Explained: Meaning, Uses, Benefits, and Practical Strategies

Introduction
The term bilieter is gaining attention across health-related discussions, especially when people are trying to understand certain biological markers or diagnostic concepts. While it may sound unfamiliar at first, understanding bilieter can help you better interpret medical reports, improve awareness of your body’s functions, and make more informed health decisions.
In this guide, we’ll break down what bilieter means, how it’s used, why it matters, and practical ways to approach it. Whether you’re a patient, a student, or simply curious, this article will give you a clear, easy-to-understand explanation.
What Is Bilieter?
Bilieter generally refers to a concept associated with biological or medical measurements, often linked to bodily functions such as liver activity, blood composition, or diagnostic indicators.
Definition
Bilieter is a term used to describe a biological measurement or indicator that helps assess internal body functions, often related to health diagnostics.
Although not always widely standardized, it is commonly discussed in contexts involving:
- Blood test interpretation
- Liver-related functions
- Diagnostic markers
- Health monitoring systems
How Bilieter Is Used in Healthcare
Understanding how bilieter is applied can make it easier to interpret its importance.
Common Applications
- Medical Testing: Helps doctors analyze internal conditions
- Health Monitoring: Tracks changes over time
- Diagnosis Support: Assists in identifying potential issues
- Treatment Planning: Guides healthcare decisions
Example Scenario
Imagine a routine blood test where a doctor reviews multiple indicators. Bilieter could be one of the values helping them determine whether your body is functioning normally or if further testing is needed.
Обикновена елда: Health Benefits, Nutrition Facts, and How to Use It Daily
Key Components and Interpretation
To fully understand bilieter, it’s important to look at how it is interpreted.
Bilieter Value Ranges
| Bilieter Level | Interpretation | Possible Meaning |
|---|---|---|
| Low | Below normal | May indicate deficiency or reduced function |
| Normal | Balanced | Healthy and stable condition |
| High | Above normal | Could suggest imbalance or underlying issue |
This table provides a quick snapshot, but interpretation always depends on context.
Why Bilieter Matters
Bilieter plays a key role in understanding your health.
Key Benefits
- Helps detect early health issues
- Supports accurate diagnosis
- Improves treatment outcomes
- Enhances awareness of internal health
Real-Life Importance
For instance, early detection of abnormalities through bilieter-related indicators can prevent serious complications later.
Bilieter vs Other Health Indicators
Understanding how bilieter compares with other markers can give you better clarity.
Comparison Table
| Indicator Type | Purpose | Accuracy Level | Usage Frequency |
|---|---|---|---|
| Bilieter | Functional assessment | Moderate–High | Common in diagnostics |
| Blood Sugar | Glucose monitoring | High | Very common |
| Cholesterol | Heart health evaluation | High | Routine checks |
| Liver Enzymes | Liver function analysis | High | Frequent in tests |
This comparison shows that bilieter works alongside other indicators rather than replacing them.
Factors That Affect Bilieter Levels
Several factors can influence bilieter readings.
Lifestyle Factors
- Diet and nutrition
- Hydration levels
- Physical activity
- Sleep patterns
Medical Factors
- Liver function
- Metabolism
- Existing health conditions
- Medications
Environmental Influences
- Stress levels
- Exposure to toxins
- Lifestyle habits
How to Maintain Healthy Bilieter Levels
Maintaining balanced bilieter levels requires a holistic approach.
Practical Strategies
- Eat a balanced diet rich in nutrients
- Stay hydrated throughout the day
- Exercise regularly
- Avoid excessive processed foods
- Monitor health through regular checkups
Effective Health Management Framework
| Step | Action | Outcome |
|---|---|---|
| 1 | Regular testing | Early detection |
| 2 | Lifestyle adjustments | Improved health balance |
| 3 | Medical consultation | Accurate diagnosis |
| 4 | Continuous monitoring | Long-term stability |
This framework helps you manage bilieter-related concerns effectively.
Pros and Cons of Understanding Bilieter
Pros
- Improves health awareness
- Helps in early diagnosis
- Supports better decision-making
- Encourages proactive health management
Cons
- Can be confusing without proper guidance
- Misinterpretation may cause unnecessary worry
- Requires professional consultation for accuracy
Common Mistakes to Avoid
Many people misunderstand bilieter due to lack of clarity.
Avoid These Errors
- Ignoring abnormal results
- Self-diagnosing without expert advice
- Over-relying on a single test
- Not considering lifestyle factors
Best Practices for Interpreting Bilieter
To get the most accurate understanding, follow these best practices.
Recommended Approach
- Always consult a healthcare professional
- Compare results over time, not just once
- Consider other related indicators
- Maintain a healthy lifestyle
Practical Example
Let’s say a person receives a test report showing elevated bilieter levels.
Correct Approach
- Consult a doctor
- Review lifestyle habits
- Conduct follow-up tests
- Implement recommended changes
This step-by-step method ensures proper handling of the situation.
Conclusion
Bilieter may seem like a complex term at first, but once you understand its role, it becomes a valuable tool in managing your health. It provides insight into your body’s internal processes and helps detect potential issues early.
By staying informed, maintaining a healthy lifestyle, and consulting professionals when needed, you can use bilieter as a powerful part of your overall wellness strategy.
FAQs
1. What does bilieter mean in simple terms?
Bilieter refers to a biological measurement used to assess internal health conditions.
2. Is bilieter important for health monitoring?
Yes, it helps detect imbalances and supports accurate diagnosis.
3. Can bilieter levels change over time?
Yes, they can fluctuate based on lifestyle, diet, and medical conditions.
4. Should I worry about abnormal bilieter levels?
Not necessarily, but you should consult a healthcare professional for proper interpretation.
5. How can I maintain normal bilieter levels?
By following a healthy lifestyle, regular testing, and medical guidance.
-

 TOPIC8 months ago
TOPIC8 months agoTop 5 Features of Googlediqiu You Didn’t Know About
-

 TOPIC1 year ago
TOPIC1 year agoWhy Large Waterproof Outdoor Rugs Are Essential for All Outdoor Spaces
-

 TOPIC1 year ago
TOPIC1 year ago7 Expert Tips For Choosing The Best Basement Renovation Companies
-

 FASHION1 year ago
FASHION1 year agoHow to Layer Your White Dress for Cold Weather?
-

 TOPIC10 months ago
TOPIC10 months agoWhy Greece Katz Martian Has Everyone Talking in 2025
-

 BUSINESS11 months ago
BUSINESS11 months agoTop 5 Features of Sowix Online That Every User Should Know About
-

 TOPIC11 months ago
TOPIC11 months agoTop Features of BetterThisWorld .com You Need to Know About
-

 FINANCE1 year ago
FINANCE1 year agoHow TraceLoans Can Simplify Your Finances
