HEALTH
Reducing Provider Burnout: How Concurrent Coding and Risk Adjustment Software Streamline Workflows

The Burden of Documentation: A Physician’s Daily Struggle
Dr. Emily Matthews wraps up her last patient visit of the day, but instead of heading home, she sits at her desk for hours, catching up on unfinished notes. The electronic health record (EHR) system stares back at her, reminding her of pending diagnoses, coding clarifications, and compliance checks. She sighs, knowing that the administrative burden is stealing precious time from her personal life and adding to her exhaustion.
Dr. Matthews’ experience is not unique. Studies indicate that physicians spend up to 50% of their workday on EHR tasks and documentation, often extending into after-hours work, commonly known as “pajama time.” The overwhelming load of retrospective coding, compliance pressures, and administrative work contributes significantly to provider burnout. But what if there was a way to integrate coding seamlessly into patient encounters and eliminate the post-visit workload?
The Link between Provider Burnout and Administrative Burden
Burnout among healthcare providers is a well-documented crisis. Excessive administrative demands not only lead to professional fatigue but also impact patient care quality. Several key factors contribute to this issue:
- Excessive Documentation: Physicians often spend more time on documentation than on direct patient care, leading to long hours and increased stress.
- Retrospective Coding Delays: The traditional approach of coding patient encounters retrospectively forces providers to recall details days or weeks later, increasing errors and frustration.
- Compliance Pressures: Inaccurate or incomplete documentation can result in claim denials, audits, and revenue loss, adding further stress to already overburdened providers.
This is where concurrent coding and risk adjustment software come into play, offering a transformative solution to these pain points.
How Concurrent Coding Eases Provider Workloads
Concurrent coding integrates coding processes into real-time patient encounters, eliminating the need for retrospective documentation. By leveraging AI-powered risk adjustment software, healthcare organizations can significantly reduce provider burden and enhance compliance.
Real-Time Documentation Minimizes After-Hours Work
With concurrent coding, physicians complete documentation during the patient visit, reducing the need to revisit notes later. This:
- Eliminates late-night EHR sessions.
- Reduces recall errors, ensuring that patient interactions remain the focus.
- Enhances efficiency, allowing physicians to see more patients without added stress.
Reduces Query Burden between Coders and Providers
Traditional retrospective coding often leads to numerous clarification requests from coders to providers, disrupting workflows. Concurrent coding:
- Enables real-time collaboration between coders and clinicians.
- Reduces the need for back-and-forth communication, minimizing disruptions.
- Streamlines workflow by ensuring documentation completeness at the point of care.
Enhances Coding Accuracy and Compliance
Capturing risk-adjusted diagnoses in real-time ensures that claims are coded accurately, reducing:
- Denials due to incomplete or inaccurate documentation.
- Compliance risks associated with incorrect coding practices.
- Provider stress linked to reimbursement challenges.
The Role of Risk Adjustment Software in Streamlining Workflows
Beyond concurrent coding, AI-powered risk adjustment software plays a critical role in automating documentation accuracy, improving compliance, and preventing revenue loss. Platforms like Algocademy, which specialize in AI-driven solutions for healthcare documentation and compliance, offer valuable tools that align with these goals by enhancing real-time coding accuracy and streamlining provider workflows.
AI-Powered Code Capture for Immediate Documentation
Risk adjustment software can automatically extract diagnoses and map them to Hierarchical Condition Category (HCC) codes while providers document notes. This:
- Reduces manual data entry errors.
- Ensures accurate reimbursement for risk-adjusted conditions.
- Enhances clinical documentation integrity.
Seamless Integration with EHR Systems
Advanced solutions embed coding prompts within EHRs, reminding providers of necessary risk-adjusted conditions in real time. This:
- Reduces the need for manual searches.
- Improves the likelihood of capturing all necessary diagnoses during the patient visit.
- Helps providers comply with CMS risk adjustment coding standards.
Predictive Analytics for Proactive Risk Adjustment
Risk adjustment software identifies missing diagnoses and suggests corrections before claims submission. This:
- Reduces coding errors.
- Ensures complete documentation, preventing future audits.
- Strengthens financial performance for healthcare organizations.
Automated Compliance Audits to Reduce Documentation Stress
By running compliance checks before claim submission, AI-driven risk adjustment software:
- Identifies coding discrepancies early.
- Reduces provider involvement in audits.
- Ensures smooth and accurate claim processing.
The Tangible Benefits of Adopting Concurrent Coding and Risk Adjustment Software
- Less Documentation Burden on Providers: Reduces after-hours work and administrative fatigue.
- Higher Revenue Capture: Ensures all risk-adjusted conditions are correctly documented, leading to optimized reimbursements.
- Stronger Compliance and Reduced Audit Risks: Minimizes coding errors that lead to payment clawbacks and compliance penalties.
- More Time for Patient Care: Allows physicians to focus on quality interactions rather than battling documentation fatigue.
Best Practices for Implementing Concurrent Coding and Risk Adjustment Software
Train Providers on Real-Time Documentation Best Practices
- Help clinicians adapt to concurrent coding workflows.
- Reinforce financial and compliance benefits of accurate coding.
Integrate AI-Driven Risk Adjustment Software
- Use predictive analytics to identify missing risk-adjusted conditions before claim submission.
- Automate real-time coding assistance to prevent coding errors.
Monitor Key Performance Indicators (KPIs) on Burnout Reduction
- Track time saved on documentation.
- Assess reductions in coding queries and provider satisfaction trends.
Align Risk Adjustment Strategies with Value-Based Care Models
- Ensure risk coding supports preventive care initiatives rather than just financial goals.
- Optimize workflows to balance reimbursement accuracy with clinician well-being.
Encourage Collaboration between Providers, CDI Teams, and Coders
- Establish real-time communication channels for seamless integration.
- Reduce friction in the documentation process through shared data insights.
The Future of Burnout Prevention through Automation
- Advancements in AI-Driven Coding Assistance: Machine learning will further enhance real-time documentation and workflow efficiency.
- Deeper Integration with EHR Systems: Risk adjustment software will become fully embedded in clinical workflows.
- Greater Focus on Clinician Well-Being: Future solutions will prioritize reducing administrative fatigue and improving physician work-life balance.
Actionable Steps for Healthcare Leaders
- Assess Provider Workloads and identify documentation pain points.
- Adopt AI-Driven Risk Adjustment Software to reduce manual coding burden.
- Develop a Real-Time Documentation Strategy centered on concurrent coding.
- Measure Workflow Optimization Impact on burnout and financial performance.
Conclusion
Concurrent coding and AI-powered risk adjustment software are no longer optional—they are essential solutions for reducing provider burnout, optimizing workflows, and improving documentation accuracy. By integrating these technologies, healthcare organizations can create a smoother, more efficient system where providers spend less time on paperwork and more time doing what they do best—caring for patients.
HEALTH
Unraveling the Benefits of FiberNL: A Comprehensive Guide

Introduction to FiberNL
Are you feeling a little sluggish lately? Struggling with digestion or trying to shed those extra pounds? If so, it might be time for a fiber boost. Enter FiberNL—a revolutionary supplement designed to enhance your overall health and wellness. Packed with essential nutrients, FiberNL is not just another addition to the endless list of dietary supplements; it’s a game-changer in how we think about fiber intake.
In our fast-paced world, many people overlook the importance of fiber in their diets. Yet this vital component plays a crucial role in maintaining good health. So, what exactly can FiberNL do for you? Join us as we unravel its benefits and explore why this innovative product should have a place in your pantry!
Understanding the Role of Fiber in Our Body
Fiber plays a crucial role in our digestive health. It acts as a natural broom, sweeping through the intestines and helping to keep everything moving smoothly. This is essential for preventing constipation and promoting regular bowel movements.
Moreover, fiber can help maintain a healthy gut microbiome. The beneficial bacteria in our guts thrive on fiber-rich foods, contributing to overall health and immunity.
There are two types of fiber: soluble and insoluble. Soluble fiber dissolves in water, forming a gel-like substance that can aid in lowering cholesterol levels. Insoluble fiber adds bulk to stool and helps food pass more quickly through the stomach.
Including enough fiber in your diet supports not just digestion but also offers protective benefits against various diseases such as diabetes and heart disease. It’s clear that embracing dietary fiber enhances both well-being and vitality at every stage of life.
What Makes FiberNL Different from Other Fiber Supplements?
FiberNL stands out in the crowded market of fiber supplements due to its unique formulation. Unlike many other products, FiberNL combines both soluble and insoluble fibers. This dual approach ensures comprehensive digestive support.
Its sourcing is also noteworthy. FiberNL utilizes natural ingredients that are non-GMO and free from artificial additives. This commitment to quality resonates with health-conscious consumers looking for clean labels.
Another significant aspect is its enhanced absorption technology. This innovation allows your body to utilize the nutrients effectively, maximizing benefits while minimizing waste.
Many users report a smoother integration into their daily routine compared to conventional fiber options. The taste profile is mild, making it versatile for mixing into various dishes or beverages seamlessly without altering flavor significantly.
The emphasis on promoting gut health sets FiberNL apart as well, supporting not only digestion but overall wellness through a balanced microbiome environment.
The Benefits of Taking FiberNL:
Taking FiberNL can significantly improve digestion and promote regularity. Many users report feeling lighter and more comfortable after incorporating it into their routines. This fiber supplement supports a healthy gut, making those occasional digestive issues less likely.
Lowered cholesterol levels are another remarkable benefit of FiberNL. Research suggests that soluble fibers found in this product can help reduce bad cholesterol, contributing to better heart health. It’s a simple way to support your cardiovascular system while enjoying other dietary benefits.
For those managing weight, FiberNL is a game-changer. It helps you feel fuller for longer, which can curb unnecessary snacking between meals. When combined with a balanced diet, this natural fiber source aids in achieving weight loss or maintenance goals effectively.
In essence, incorporating FiberNL offers an array of advantages that enhance both your physical well-being and quality of life.
– Improved Digestion and Regularity
A healthy digestive system is crucial for overall well-being, and FiberNL plays a significant role in this. By providing the right amount of soluble and insoluble fiber, it supports optimal gut health.
Fiber helps to bulk up stool, making it easier to pass through the intestines. This can lead to improved regularity and reduced discomfort associated with constipation.
Many users have reported feeling lighter and more energetic after incorporating FiberNL into their daily routine. The gentle yet effective nature of its ingredients ensures that your body adapts without any harsh side effects.
Moreover, a balanced fiber intake can foster beneficial bacteria in your gut. These friendly microbes contribute to better digestion while also enhancing nutrient absorption from foods you consume.
With consistent use, FiberNL encourages not just comfort but also promotes a sense of overall vitality that many people crave in their busy lives.
– Lowered Cholesterol Levels
FiberNL plays a significant role in managing cholesterol levels. Soluble fiber, found in this supplement, binds to cholesterol in the digestive system. This process helps remove excess cholesterol from the body.
When you incorporate FiberNL into your routine, you may notice improvements in your lipid profile. Regular intake can lead to lower LDL (bad) cholesterol while supporting higher HDL (good) cholesterol levels.
The heart benefits immensely from healthy cholesterol management. With reduced LDL levels, the risk of cardiovascular diseases diminishes significantly.
Many people overlook fiber’s impact on heart health; however, it is vital for maintaining optimal wellness. By choosing FiberNL, you’re not just adding a supplement but enhancing your overall quality of life through better heart function and well-being.
– Weight Management
FiberNL plays a significant role in weight management. By incorporating this fiber supplement into your daily routine, you can help control your appetite more effectively.
Fiber has a unique ability to create a feeling of fullness. This means you’re likely to eat less during meals and avoid unnecessary snacking throughout the day. When combined with a balanced diet, FiberNL can be a powerful ally in achieving your weight loss goals.
Additionally, high-fiber foods take longer to digest. This slow digestion process helps stabilize blood sugar levels, reducing sudden cravings that often lead to overeating.
For those looking for sustainable weight management solutions, FiberNL offers an easy way to add essential nutrients without extra calories. The result is not just about losing pounds; it’s also about fostering healthier eating habits over time.
How to Incorporate FiberNL into Your Diet
Incorporating FiberNL into your diet is simple and versatile. Start by adding it to your morning routine. Mix a scoop with yogurt or smoothie for a fiber boost that keeps you energized.
For lunch, try sprinkling FiberNL on salads or stirring it into soups. The mild flavor won’t alter the taste but will enhance the nutritional profile of your meals.
Baking enthusiasts can experiment too. Blend FiberNL into muffin batter or homemade bread recipes for added texture and health benefits.
Even snacks can benefit! Stir some into nut butter before spreading it on whole-grain toast or apples for a satisfying treat packed with nutrients.
Listen to your body; adjust serving sizes as needed. Gradually increase intake to avoid digestive discomfort, allowing your system to adapt seamlessly to this powerful supplement.
Real Life Success Stories with FiberNL
Many people have experienced transformative results with FiberNL. Take Sarah, for instance. After struggling with digestion issues for years, she decided to give FiberNL a shot. Within just a few weeks, her bloating diminished and regularity improved significantly.
Then there’s Mark, who was battling high cholesterol levels. He incorporated FiberNL into his daily routine and was thrilled to find that his numbers began to drop after only a couple of months. The added fiber made all the difference in managing his heart health.
Jenna turned to FiberNL during her weight loss journey. By adding it to smoothies and snacks, she felt fuller longer and found it easier to resist unhealthy cravings. Her energy soared as the pounds melted away.
These stories highlight how FiberNL can make a real impact on everyday lives by addressing various health concerns effectively.
Potential Side Effects and Precautions
While FiberNL offers numerous benefits, it’s essential to be aware of potential side effects. Some individuals may experience gastrointestinal discomfort initially, such as bloating, gas, or cramping. These symptoms often improve as the body adjusts.
Hydration plays a crucial role when increasing fiber intake. Insufficient water consumption can lead to constipation instead of relief. Aim for adequate fluid intake throughout the day.
It’s wise to consult with a healthcare professional before starting any new supplement regimen, especially if you have pre-existing health conditions or are pregnant and breastfeeding.
Remember that moderation is key. Gradually introducing FiberNL into your diet allows your digestive system time to adapt while minimizing unwanted side effects.
Conclusion: Why You Should Add FiberNL to Your
FiberNL stands out as a remarkable addition to your diet if you’re looking to enhance your overall health. This unique supplement offers numerous benefits, including improved digestion and regularity, lowered cholesterol levels, and effective weight management.
Incorporating FiberNL into your daily routine is simple. Whether you mix it into smoothies or sprinkle it on meals, the versatility makes it easy to enjoy its advantages. Plus, countless real-life success stories highlight how FiberNL has transformed lives by promoting better digestive health and aiding in weight control.
While it’s essential to be aware of potential side effects like bloating or gas for some individuals, many find that these are minor compared to the vast benefits they experience. As with any supplement, consulting with a healthcare provider before starting is always wise.
Adding FiberNL can serve as an important step toward achieving optimal health. With fiber playing such a crucial role in our well-being, embracing this supplement could lead you down a path of noticeable improvements in how you feel every day.
HEALTH
How Preventive Dental Care Shapes Lifelong Oral Health

Achieving and maintaining a healthy smile is much more than a cosmetic concern. Oral health serves as a vital foundation for one’s overall wellness by influencing numerous aspects of daily life, from nutrition to self-confidence. Preventive dental care offers a pathway to protecting your teeth and gums against disease and infection. With routine dental checkups and proper home care, people can help avoid future dental complications, potentially costly treatment, and maintain strong oral health for years to come. For those considering restorative options, learning about affordable dental implants can also be a valuable step towards improving their dental health and quality of life.
Investing in preventive care not only leads to brighter smiles but also supports long-term health. Taking proactive steps, such as adopting consistent oral hygiene habits and seeking regular dental visits, empowers individuals to catch issues early. This approach helps reduce risks for more complex procedures and supports lasting comfort and well-being.
The Importance of Regular Dental Check-Ups
Routine appointments with a dental professional serve as a crucial line of defense against serious oral health concerns. Dental checkups typically involve a thorough examination of the teeth and gums, professional cleanings, and sometimes diagnostic X-rays to uncover hidden concerns. When issues like early-stage cavities or the beginning signs of gum disease are found, dentists can provide prompt and effective treatment, helping patients avoid more advanced dental conditions or expensive interventions down the road.
Daily Oral Hygiene Practices
Maintaining optimal oral health begins with simple habits practiced every day. Brushing at least twice daily with fluoride toothpaste and flossing once a day are fundamental components of any preventive routine. These actions help to remove plaque, a film of bacteria, setting the stage for tooth decay and gum disease. Supplementing brushing and flossing with an antimicrobial mouthwash can further reduce bacteria and contribute to fresher breath.
Fluoride Treatments and Dental Sealants
Fluoride is well known for its ability to strengthen tooth enamel, offering vital protection against cavities. While fluoride is commonly added to public water supplies, some individuals may benefit from additional fluoride treatments during dental visits, particularly children, adolescents, and those with heightened cavity risk. Dental sealants provide another effective preventive strategy. By applying a thin, protective layer to the chewing surfaces of molars, sealants can block out food and bacteria, significantly lowering the likelihood of tooth decay among children and teens.
Healthy Diet and Lifestyle Choices
What you consume can have a lasting impact on your dental health. A diet packed with fresh produce, lean proteins, and whole grains delivers essential nutrients that keep teeth and gums resilient. Reducing your intake of sugary foods and beverages helps guard against cavities. Habits such as avoiding tobacco and limiting alcohol use are also critical for preventing oral cancers and supporting ongoing dental health.
Addressing Dental Anxiety
Many individuals experience unease or even fear when visiting the dentist. Dental anxiety can impede the pursuit of necessary preventive care, potentially leading to neglected oral health. Open communication with your dental provider about your concerns is vital. Modern dental offices offer solutions from sedation dentistry to relaxation and coping techniques. These options can transform the dental experience, making it easier to attend regular visits and receive needed care with greater comfort.
The Link Between Oral and Overall Health
Oral health extends beyond the mouth, with research increasingly revealing links to wider systemic conditions. Issues such as poor gum health and untreated cavities have been associated with increased risks for heart disease, diabetes, and respiratory infections. Conversely, diligent oral hygiene can help protect against these serious health concerns. A recent study reported by Fox News highlighted that maintaining a simple and consistent brushing routine may also contribute to reducing dementia risk and other related conditions.
Overcoming Barriers to Preventive Care
Despite the clear benefits, obstacles like financial constraints, lack of transportation, or limited education about oral health can prevent individuals from receiving regular care. Community-based programs, mobile dental units, and sliding-fee structures have emerged to address these challenges and make services more accessible. Public awareness campaigns and outreach efforts are also essential to educate people about the importance of preventive dental care and the resources available to them. For example, initiatives discussed in a World Health Organization article demonstrate how targeted strategies can improve oral health outcomes in local communities.
Adopting a proactive approach to preventive dental care sets a foundation for lifelong oral health. Through regular dental visits, dedicated home care, and mindful lifestyle habits, everyone can work toward a confident smile and enhanced well-being at every age.
HEALTH
What to Know Before Getting Dental Implants
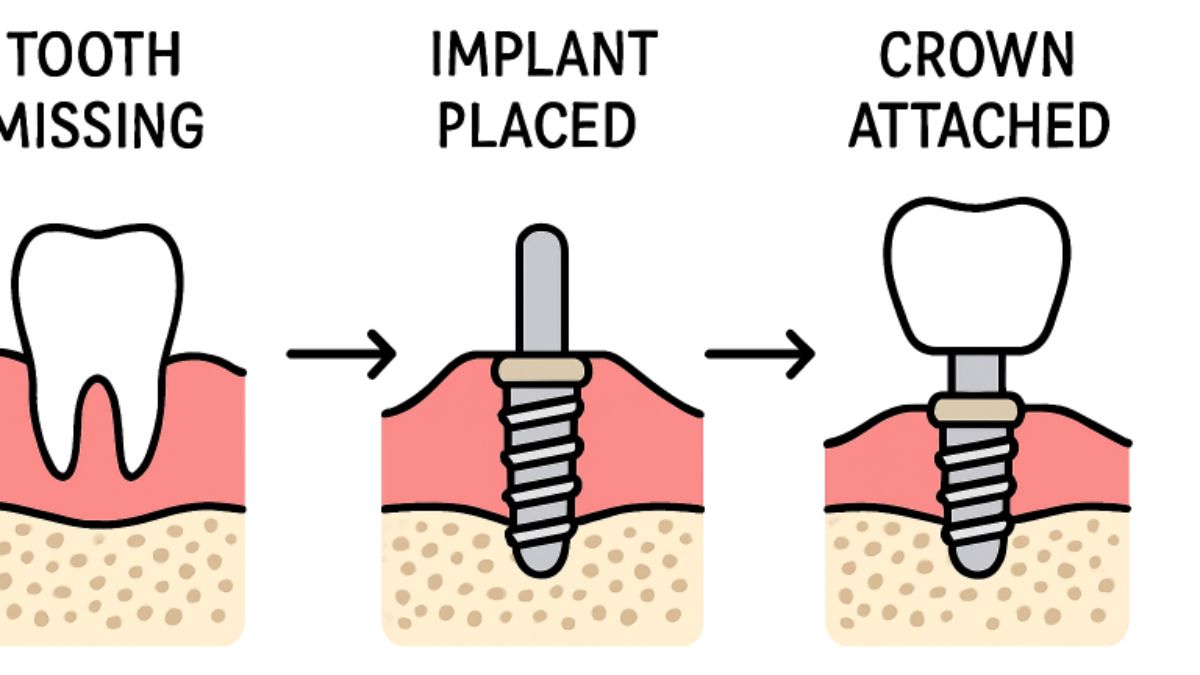
Dental implants have transformed restorative dentistry by providing a durable, comfortable, and natural-looking solution for replacing missing teeth. Many individuals are considering options such as denture implants to regain their confidence and oral function. However, questions often arise regarding implant procedures, candidacy, potential risks, and costs. Understanding clear answers to these questions can help you make a decision that’s right for your dental health. When deciding between dentures and implants, it’s important to understand what each treatment involves, the recovery time required, and which option best fits your specific needs and lifestyle. Dental professionals frequently address concerns about pain, longevity, daily maintenance, and how implants compare to traditional options. If you’re considering dental implants, obtaining accurate, up-to-date information is crucial for a smooth treatment experience and satisfying results.
What Are Dental Implants?
Dental implants function as artificial tooth roots, typically made from medical-grade titanium. These posts are surgically placed into the jawbone, where they integrate with your bone tissue in a process called osseointegration. After the implant is stable, a connector and a custom crown are attached, resulting in a secure, natural-looking tooth replacement. Dental implants are customized to match the color and shape of your natural teeth, ensuring a seamless blend within your smile.
Who Is a Suitable Candidate for Dental Implants?
Candidates for dental implants need healthy gums, no untreated dental conditions, and sufficient jawbone density to support the dental implant post. Factors such as smoking, uncontrolled diabetes, or ongoing periodontal disease can negatively impact healing and the success of the procedure. Before treatment, your dentist will conduct a thorough screening to ensure that implants are a safe and effective option for you.
What Does the Implant Procedure Involve?
The procedure for placing dental implants involves several stages, each crucial for the long-term success of your new teeth:
- Initial Consultation: Your dental provider will evaluate your oral health, review your medical history, and take digital scans or X-rays to assess jawbone strength.
- Surgical Placement: The titanium post is surgically positioned within the jawbone under local anesthesia. This step forms the stable foundation for your future restoration.
- Healing and Osseointegration: Over several months, the implant fuses with your jawbone, a vital process that ensures stability and prevents bone loss.
- Abutment Placement: After healing, a small connector (abutment) is attached to the implant to hold the crown in place.
- Crown Attachment: A custom-made crown is affixed to the abutment, completing the restoration and restoring full function and appearance.
How Long Do Dental Implants Last?
Dental implants are designed for longevity and, with proper care, can last a lifetime. The implant itself is typically permanent, though the crown may need to be replaced after 10 to 15 years due to normal wear. Consistent oral hygiene, avoiding smoking, and regular dental visits all contribute to the long-term success of dental implants.
Are Dental Implants Painful?
Most patients find dental implant procedures less uncomfortable than anticipated. During surgery, local anesthesia minimizes pain, and any post-operative discomfort is usually mild and short-lived. Over-the-counter pain medications or prescribed analgesics are generally effective during the initial healing period. After a few days, most individuals can return to their usual routines without significant discomfort.
What Are the Advantages of Dental Implants?
- Durability: Implants can last for several decades if cared for properly, making them a cost-effective, long-term solution.
- Natural Appearance: The design of implants mimics real teeth in both look and function, giving a seamless, attractive smile.
- Bone Preservation: By stimulating jawbone growth, implants prevent the bone loss commonly seen after tooth extraction.
- Enhanced Chewing Function: Unlike removable dentures, implants allow you to eat a wide variety of foods with confidence.
These benefits often give dental implants an edge over traditional bridges or dentures, especially for those seeking lifelong oral health improvements.
What Are the Potential Risks or Complications?
While dental implant success rates are high, complications can occur. Risks include infection around the implant site, implant failure (rare but more likely in smokers), injury to nerves near the jaw, or sinus issues with implants placed in the upper jaw. Choosing a skilled dental specialist, following post-care instructions, and maintaining excellent oral hygiene are the best ways to minimize these risks. For detailed information on potential risks, refer to the FDA’s guidelines on dental implants.
How Much Do Dental Implants Cost?
The overall price of dental implants depends on the number of implants needed, the type of restoration, pre-existing oral health conditions, and location. Typically, one implant with a crown will cost between $3,000 and $5,000. Dental insurance plans may partially cover the expense, but many policies still categorize implants as elective or cosmetic. Discussing options with both your provider and insurer can clarify out-of-pocket expenses and payment plans.
Conclusion
Dental implants are a reliable, innovative solution for restoring missing teeth and enhancing your oral health, function, and confidence. Knowing what to expect before, during, and after the procedure will help you make a decision tailored to your unique needs. For all individual considerations, work closely with a trusted dental professional who can guide you through the process and help achieve lasting results.
-

 TOPIC9 months ago
TOPIC9 months agoTop 5 Features of Googlediqiu You Didn’t Know About
-

 TOPIC1 year ago
TOPIC1 year agoWhy Large Waterproof Outdoor Rugs Are Essential for All Outdoor Spaces
-

 TOPIC2 years ago
TOPIC2 years ago7 Expert Tips For Choosing The Best Basement Renovation Companies
-

 FASHION2 years ago
FASHION2 years agoHow to Layer Your White Dress for Cold Weather?
-

 TOPIC11 months ago
TOPIC11 months agoWhy Greece Katz Martian Has Everyone Talking in 2025
-

 BUSINESS12 months ago
BUSINESS12 months agoTop 5 Features of Sowix Online That Every User Should Know About
-

 TOPIC12 months ago
TOPIC12 months agoTop Features of BetterThisWorld .com You Need to Know About
-

 FINANCE1 year ago
FINANCE1 year agoHow TraceLoans Can Simplify Your Finances
